Coagulation
| Home | | Pharmacology |Chapter: Essential pharmacology : Drugs Affecting Coagulation, Bleeding And Thrombosis
Haemostasis (arrest of blood loss) and blood coagulation involve complex interactions between the injured vessel wall, platelets and coagulation factors.
COAGULATION
Haemostasis (arrest of blood loss) and blood coagulation involve
complex interactions between the injured vessel wall, platelets and coagulation
factors. A cascading series of proteolytic reactions (Fig. 44.1) is started by:
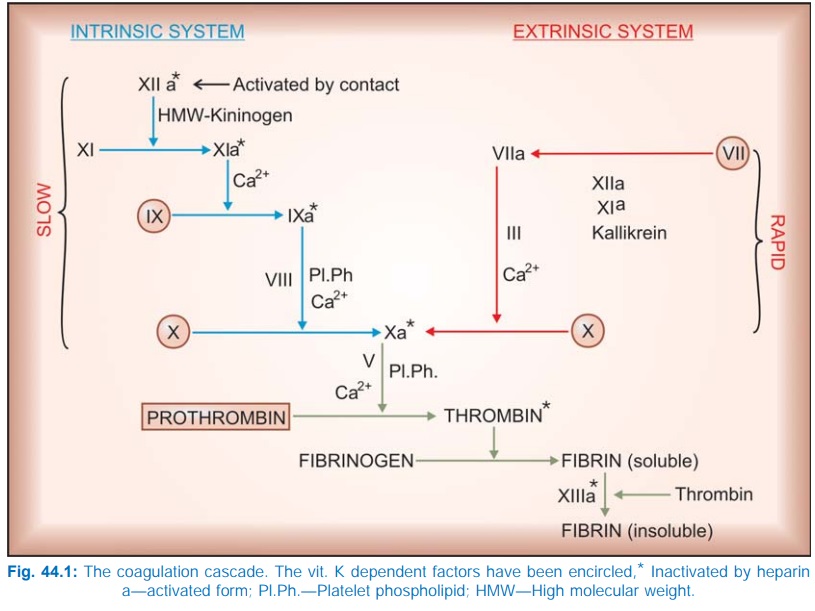
i) Contact activation
of Hageman factor: intrinsic system,
in which all factors needed for coagulation
are present in plasma. This is slow and takes several minutes to activate
factor X.
ii) Tissue thromboplastin: extrinsic system, needs a tissue
factor, but activates factor X in seconds.
The subsequent events are common in the two systems and result
in polymerization of fibrinogen to form fibrin strands. Blood cells are trapped
in the meshwork of fibrin strands producing clot.
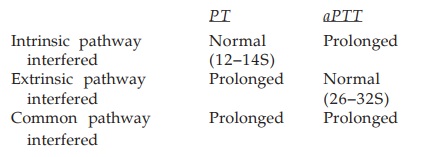
Two in vitro
tests ‘activated partial thromboplastin time’ (aPTT) and ‘prothrombin time’
(PT) are employed for testing integrity of the intrinsic, extrinsic and common
pathways of the coagulation cascade. The results are interpreted as:

Most clotting factors
are proteins present in plasma in the inactive (zymogen) form. By partial
proteolysis they themselves become an active protease and activate the next
factor. In addition to its critical role in cleaving and polymerizing
fibrinogen, thrombin activates many upstream factors (especially f. XI, VIII
and V) of the intrinsic and common pathways—amplifying its own generation and
continuation of clot formation. It is also a potent activator of platelets.
On the other hand,
factors like antithrombin, protein C, protein S, antithromboplastin and the fibrinolysin system tend to oppose coagulation and lyse formed clot. Thus, a check and
balance system operates to maintain blood in a fluid state while in circulation
and allows rapid haemostasis following injury.
